Introduction: Self-Inflicted Ingestion in Psychiatric Patients
The phenomenon of intentionally ingesting foreign objects poses a significant challenge in today’s healthcare landscape. Particularly, patients with psychiatric conditions often find themselves caught in a cycle of self-harming behavior that leads to recurrent episodes of foreign body ingestion. This opinion editorial aims to examine one such case and discuss the tricky parts of managing these situations, especially from a conservative management perspective.
In this discussion, we will poke around various treatment strategies, weigh the pros and cons of surgical intervention versus non-invasive observation, and emphasize a multidisciplinary approach. By taking a closer look at both the clinical and psychological dimensions, we hope to provide a balanced, neutral view on a subject that is too often seen as overwhelming and off-putting.
Understanding the Tangled Issues Behind Recurrent Ingestion
On many levels, recurrent foreign body ingestion in psychiatric patients is riddled with tension and full of problems that test the limits of both medical expertise and mental health support. Patients who repeatedly ingest objects like nails often suffer from disorders such as borderline personality disorder and bipolar affective disorder. These cases are not only medically challenging but also socially and emotionally loaded with issues.
Some of the confusing bits when managing these patients include:
- Identifying the motivations behind the self-harming behavior
- Evaluating the risk for immediate gastrointestinal complications
- Deciding between invasive (surgical) and non-invasive (conservative) approaches
- Managing the triggers that lead to repeated episodes
As clinicians try to figure a path through these tangled issues, it becomes essential to balance effective medical care with continuous psychiatric support. Each element of the case—from imaging findings to the patient’s mental health history—plays a critical role in deciding how best to make progress without adding undue risk.
Conservative Versus Surgical Management: Weighing the Options
The management of foreign body ingestion is a choice between pursuing immediate surgical intervention and adopting a conservative strategy based on careful clinical observation. In cases where multiple foreign bodies are ingested over time, history becomes laden with previous surgeries that contribute to a hostile abdomen. This is characterized by tangled adhesions and other complications that make another surgery not just intimidating but potentially nerve-racking.
Reasons to Prefer Conservative Management
When faced with a patient who is clinically stable and without acute signs of complications such as perforation or sepsis, a conservative approach may be appropriate. Some of the key reasons to opt for non-invasive management include:
- Reduced Surgical Risks: Repeated surgeries can lead to extensive adhesions, increasing the likelihood of post-operative complications.
- Clinical Stability: Patients who remain stable and show no signs of internal bleeding or perforation may benefit from thorough observation.
- Progression Monitoring: Serial imaging techniques, like plain radiographs and CT scans, enable physicians to monitor the migration of the ingested objects without an immediate invasive procedure.
- Improved Recovery: Non-surgical management can potentially lead to a shorter hospital stay and reduce the burden of post-operative recovery.
This method is not without its challenges, however. The conservative strategy requires vigilant monitoring and quick decision-making should the patient’s clinical picture worsen. By sorting out the treatment plan based on constant re-assessment, clinicians can ensure that if subtle signs point toward complications, surgical intervention can be swiftly initiated.
Risks and Benefits of Surgical Intervention
Surgical removal of ingested objects is often seen as a direct solution to eliminate the risk of ongoing damage to the gastrointestinal tract. However, surgery in these cases is a double-edged sword. The benefits and tricky parts include:
- Benefits:
- Immediate removal of dangerous objects
- Direct visualization of the gastrointestinal tract, which can help in addressing unnoticed injuries
- Challenges:
- The potential for a hostile abdomen with extensive adhesions
- Increased risk for complications such as infection, perforation, and prolonged recovery time
- Possible repeated surgeries if the behavior continues over time
Thus, the decision to operate on a patient with recurrent self-harm through ingestion must be made carefully. When clinical indicators and radiological imaging do not point toward immediate danger, conservative management can be safely pursued, with the constant readiness to change the strategy if the situation turns tense.
Case Reflection: A Closer Look at a Real-Life Instance
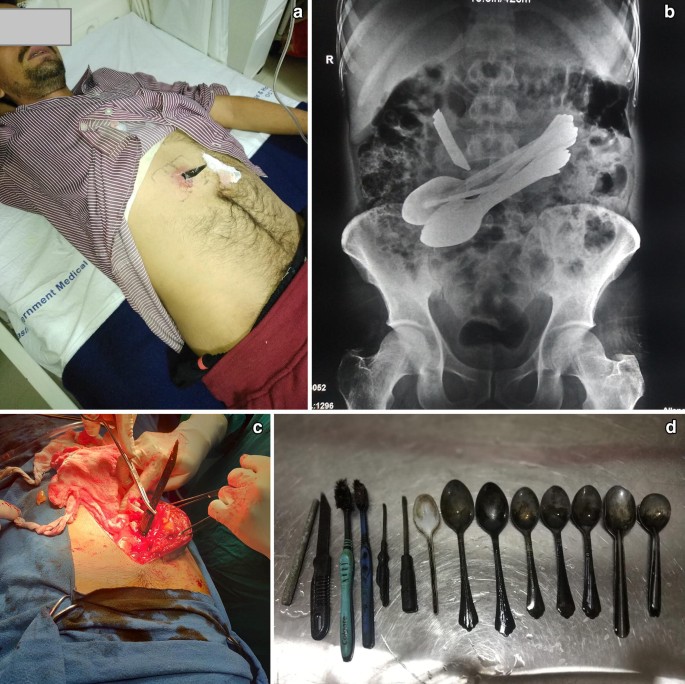
Consider the case of a 33-year-old woman diagnosed with bipolar affective disorder and borderline personality disorder. She presented with abdominal pain, melena, vomiting, and anorexia following the ingestion of several nails—a recurring behavior that had led her to undergo four prior surgical interventions. The patient’s history already painted a picture filled with numerous twists and turns.
Upon presentation at the emergency department, imaging played a critical role in understanding the situation. A supine abdominal X-ray revealed multiple radiopaque objects scattered throughout the gastrointestinal tract. Further evaluation using computed tomography (CT) confirmed widespread ingestion with evidence of mild inflammatory changes. Upper gastrointestinal endoscopy, unfortunately, did not yield any positive results for safe removal, as the sheer volume and arrangement of the nails rendered the attempt impractical.
Medical Details and Imaging Findings: Getting into the Nitty-Gritty
The imaging studies in this case serve as an example of how doctors poke around the fine points of diagnosis. These methods include:
- Plain Radiography: Used to identify the location and quantity of metallic foreign bodies.
- Computed Tomography (CT): Offers a detailed view of the gastrointestinal tract, highlights segmental wall thickening, and detects areas of fat stranding indicative of inflammation.
- Upper Gastrointestinal Endoscopy: Essential for both confirming the presence of the ingested material and assessing whether an endoscopic removal is a feasible option.
In this instance, given the patient’s extensive history of laparotomies resulting in a hostile abdomen, the decision was made to avoid surgery and adopt conservative management. This approach involved close clinical and radiological monitoring, with the expectation that the ingested nails would progress through the digestive system and be eliminated spontaneously. Over a period of 18 days, the patient showed gradual improvement, and repeated imaging confirmed the steady migration of the metallic objects without causing obstruction or perforation.
The Multidisciplinary Approach: Bringing Together Medical and Psychiatric Care
One of the most important aspects of dealing with recurrent ingestion cases is the integration of medical treatment with psychiatric support. It is not enough to simply manage the physical complications associated with the ingestion of dangerous objects; the underlying mental health issues must be addressed concurrently.
The Importance of Psychiatric Follow-Up and Therapy
A continuous and structured psychiatric follow-up is key to preventing further episodes of self-harm. In the case discussed, the patient was already under regular supervision at a psychosocial care center. Her pharmacologic management included mood stabilizers, antipsychotics, and anxiolytics, which together aimed to reduce impulsivity and self-destructive tendencies.
In addition to medication, structured psychotherapeutic approaches such as dialectical behavior therapy (DBT) have proven super important for individuals with borderline personality disorder. DBT offers strategies for coping with intense emotions and helps patients develop healthier ways of responding to stress. This dual approach—combining pharmacological intervention with behavioral therapies—can be summarized as follows:
- Pharmacological Support:
- Mood stabilizers (e.g., lithium, valproic acid)
- Antipsychotic medications (e.g., haloperidol)
- Anxiolytics (e.g., diazepam)
- Psychotherapeutic Strategies:
- Dialectical Behavior Therapy (DBT)
- Cognitive Behavioral Therapy (CBT)
- Ongoing counseling and crisis intervention
The subtle parts of a patient’s mental health condition are just as important as the concrete physical symptoms. Effective management relies on an in-depth understanding of these small distinctions to design a holistic treatment plan that addresses both mind and body.
Tackling the Tricky Parts: Fine Points in Management Strategies
One of the most delicate areas in managing recurrent foreign body ingestion is determining the balance between immediate surgical intervention and conservative care. Each treatment plan must be uniquely tailored, taking into account factors such as the patient’s surgical history, current clinical presentation, and underlying psychiatric issues.
Fine Shades of Treatment Planning
When working through a treatment strategy, practitioners must consider several fine shades of decision-making. Key elements include:
- Volume and Nature of Ingested Material: Sharp, metallic objects carry a high risk of causing damage to the gastrointestinal tract. In cases where multiple objects are involved, surgery might seem like the quicker option, yet the cumulative effect of repeated surgeries can be overwhelming.
- Significance of a Hostile Abdomen: Previous surgical interventions can lead to the formation of dense adhesions. These adhesions are hidden complexities that not only make surgical procedures more difficult but also increase the risk for further intra- and postoperative complications.
- Indicators for Conservative Management: If the patient is hemodynamically stable, without signs of perforation or sepsis, careful observation and non-invasive management can be the safer bet. Serial abdominal radiographs offer a window into the process, helping clinicians steer through the decision-making path.
It is essential to note that conservative management is not a one-size-fits-all solution. The patient’s progress must be continuously monitored, with the readiness to act should any subtle signs of deterioration arise. This approach demands a fine balance—not just between physical and psychological elements, but also between short-term safety and long-term recovery.
Risk Management Amid Previous Surgeries
Patients who have undergone multiple surgeries are confronted with additional risks when it comes to managing new episodes of foreign body ingestion. The surgical field in such cases is often described as a “hostile abdomen,” filled with tangled issues such as adhesions. The risks associated with performing another operation include:
- Infection: Repeated surgical incisions can compromise the sterile environment, making infections more likely.
- Tissue Damage: Dense adhesions increase the chances of accidental injury to surrounding organs during surgery.
- Extended Recovery Periods: Each surgery adds to the overall healing time, which can have a negative impact on the patient’s quality of life.
For these reasons, doctors and medical teams often find their way through a maze of considerations before deciding to operate again. Instead, if the patient’s status remains stable, a strategy focused on observation, analgesia, and supportive care may be the more judicious choice.
Implications for Future Care and Prevention Strategies
The challenge of recurrent foreign body ingestion is not solely a question of immediate medical management but also of implementing preventive measures for the future. Treating each incident in isolation does little to address the root causes of self-injurious behavior.
Preventive Measures and Long-Term Management
Establishing preventive strategies is key to reducing the recurrence of such risky behavior. Some suggested measures include:
- Continuous Psychiatric Care: Regular sessions with mental health professionals and ongoing crisis interventions can help address the deep-rooted psychological issues driving self-harm.
- Structured Psychotherapy Programs: Approaches like DBT provide patients with coping skills to better manage distress and reduce impulsivity.
- Family and Social Support: Incorporating family counseling and ensuring a robust support network can work wonders in preventing relapse.
- Community-Based Services: Facilities that offer a blend of psychiatric and social care, such as Psychosocial Care Centers (CAPS), are critical in providing a safety net for vulnerable patients.
By embracing these preventive measures, healthcare providers can take a proactive stance. It’s all about finding your path to not only treating the physical manifestations but also addressing the emotional triggers that lead to these repeated dangerous behaviors.
Expert Opinions and Recommendations
Leading experts in both gastroenterology and psychiatry agree that managing recurrent foreign body ingestion requires a balanced, patient-centered approach. Several important insights have emerged from the literature and clinical practice that shape current recommendations:
- Interdisciplinary Collaboration: The management of such cases is most successful when gastroenterologists, surgeons, psychiatrists, and primary care providers work in tandem.
- Individualized Risk Assessment: Every patient’s scenario contains its own set of challenges. A tailored approach that carefully weighs the risks of surgery against the benefits of conservative management is imperative.
- Regular Re-Evaluations: Continuous monitoring and re-assessment are essential. Using serial imaging studies helps clinicians make informed decisions and respond quickly to any adverse developments.
- Psychiatric and Social Interventions: Often, the long-term success of any treatment strategy depends more on sustained psychiatric engagement than on isolated medical interventions. This is vital for preventing future self-harm episodes.
Below is a summary table capturing some of the key expert recommendations:
| Aspect | Recommendation |
|---|---|
| Medical Intervention | Opt for conservative management when clinically stable; consider surgery only when absolutely necessary |
| Imaging | Use serial radiographs and CT scans for continuous monitoring |
| Psychiatric Support | Regular follow-up with mental health professionals and structured psychotherapy, like DBT |
| Preventive Strategies | Implement family support, community-based care, and tailored pharmacological treatments |
Real-Life Impacts: Balancing Medical and Emotional Outcomes
When managing cases of intentional foreign body ingestion, the patient’s physical health and emotional well-being are intricately intertwined. The decision-making process involves reviewing the subtle details of each patient’s history and current state. For instance, in our case, the patient’s stable hemodynamic profile allowed her doctors to choose an observation-focused strategy rather than an immediate surgical intervention—a decision that ultimately led to a successful outcome without added complications.
Yet, beyond the clinical markers, the overall success hinges on how well the patient is supported emotionally. This is where ongoing psychiatric care and structured psychological therapies come into play. While a conservative approach might be medically justified, its long-term success depends on addressing the recurrent nature of self-harm behaviors.
Collaborative Care as a Must-Have Strategy
It is super important to understand that no single approach will work for every individual. The following points highlight the importance of a multi-pronged strategy:
- Coordinated Communication: Regular meetings between surgeons, gastroenterologists, and mental health professionals help ensure that everyone is on the same page when a patient is being treated.
- Integrated Treatment Plans: Combining physical treatment with mental health interventions can improve overall outcomes and reduce the chance of recurrence.
- Personalized Care: Considering both the medical history and the psychological triggers of each patient allows clinicians to figure a path that is tailored to individual needs.
This multi-layered, team-based approach not only helps in smoothing out the rough edges of each treatment scenario but also offers patients a greater chance of long-term recovery and a better quality of life.
Lessons Learned and Moving Forward
The case discussed and the surrounding literature offer several lessons for clinicians grappling with the challenges of recurrent foreign body ingestion in psychiatric populations. The following are some takeaways that can help guide future practices:
- Deep Clinical Insight: Understanding the clinical presentation—whether through radiological images or close observation—is essential for making timely decisions.
- Judicious Use of Surgery: Surgical intervention should be reserved for cases where the risk of complications is high. For those patients who remain stable, non-invasive measures are often the wiser choice.
- Ongoing Psychiatric Involvement: Without addressing the underlying mental health issues, any medical intervention is merely a temporary fix. Continuous psychiatric engagement is key to breaking the cycle of self-harm.
- Preventive Measures: Emphasizing community support, family involvement, and regular mental health check-ups can help prevent future incidents.
These lessons serve as a guide, not only for managing immediate concerns but also for structuring long-term care that respects the patient’s overall well-being. In many ways, the case is a reminder that the road to recovery is a collaborative journey that must include both clinical expertise and compassionate mental health support.
Concluding Thoughts: Finding a Path Through Tangled Medical and Psychiatric Challenges
In conclusion, managing recurrent foreign body ingestion in psychiatric patients is a multifaceted undertaking filled with tricky parts and tangled issues. Through this opinion editorial, we have taken a closer look at the conservative management of such cases, weighing it against surgical intervention and emphasizing the importance of constant observation, multidisciplinary collaboration, and continuous psychiatric follow-up. The case of the 33-year-old woman, who successfully navigated an episode of massive ingestion through non-invasive care, serves as an example of how careful, patient-tailored strategies can yield positive results despite a history marked by previous complications.
While there remains no universally applicable solution, it is clear that a balanced approach—one that steers through both the physical and emotional aspects of patient care—is essential. Clinicians must remain vigilant in monitoring subtle signs of deterioration even while the patient appears stable. At the same time, the significance of psychiatric care cannot be overstated. After all, the prevention of future episodes relies heavily on addressing the underlying mental health issues that drive such behavior.
As we move forward, further research and open dialogue between surgeons, gastroenterologists, and mental health professionals will be key to unraveling the fine points of these challenging cases. It is through this collaborative effort that we can hope to improve outcomes, reduce the risks associated with repeated surgical interventions, and ultimately provide a safer, more supportive environment for our patients.
In the end, success lies in being ready to adjust one’s approach at the slightest sign of trouble—whether that means pivoting from observation to intervention or reinforcing psychiatric treatment. By continuously evaluating both the medical situation and the psychological state of the patient, healthcare providers can find their way to delivering care that is both effective and compassionate.
Final Reflections on the Way Forward
The long-term management of psychiatric patients prone to foreign body ingestion challenges clinical teams to customize their approach, combining both traditional medical interventions with innovative psychiatric therapies. Given the high stakes involved—with risks ranging from surgical complications to the deep emotional wounds of self-harm—it is critical that each case be handled with a balance of expertise, empathy, and collaboration.
While the scientific community continues to get into research on this subject, individual cases provide invaluable insights into the twists and turns inherent in treatment planning. By using imaging for continuous monitoring, opting for conservative management when possible, and ensuring rigorous psychiatric follow-up, we can stitch together a framework that benefits patients not just in the short term, but in their long-term journey toward recovery.
Healthcare is, at its core, about understanding the little details that differentiate one case from another. With recurrent foreign body ingestion, every detail—from a patient’s previous surgical history to the fine shades of their psychological state—matters. It is this attention to the nitty-gritty that informs a safer, more individualized method of care and ultimately, helps patients reclaim not only their health but their lives.
Originally Post From https://www.cureus.com/articles/388254-recurrent-foreign-body-ingestion-in-a-psychiatric-patient-a-conservative-approach
Read more about this topic at
Do conservatives really have better mental well-being than …
Why Conservatives Avoid Therapy


